T
he human body is unfathomably complex, somewhat mysterious and often fragile.
I know this because a boil nearly took my life.
In late December 2022, I developed symptoms that one might mistake for the flu or a simple infection. It began with terrible lethargy, tiredness and weakness so strong that I could hardly stay awake.
At this point in time, I had become party to a series of recent tragedies, including the deaths of my maternal grandmother, my father and my uncle, all within the span of less than a year. I was certain these events had contributed to my overall feeling of malaise. Little did I know that I was about to face another tragedy of my own.
A surprising diagnosis
The winter holidays were coming to an end. Others were preparing for the upcoming New Year celebrations, but I wasn't feeling it. I had come down with flu-like symptoms, and was too tired and too weak to care about marking the occasion.
Just days before, I had developed a small red bump protruding through the surface of my abdomen. I thought, perhaps, I was developing a boil. But the pain I felt eminating from this carbuncle was unlike anything else I had ever felt.
As I ran my fingers over my stinging skin, I noticed an unusual warmth — a sure sign of infection. The site began to develop small red streaks.
As time wore on, the pain increased. I could no longer take the discomfort.
I made my way to General’s emergency department. A young, bubbly resident performed an examination.
At first, the doctor couldn’t make sense of my symptoms. The pain I was experiencing was disproportionate to the abscess’ physical presentation. More tests were ordered.
After a series of screenings — a CT scan, a battery of blood work, continuous vital checks — an underlying diagnosis was reached. It seemed a life-threatening bacteria, naturally present on many people’s skin — mine included — had entered my body through the opening of a small boil on my abdomen.
I had developed Necrotizing fasciitis, the so-called “flesh-eating disease.”
Necrotizing fasciitis — a rare, serious, often deadly disease
The rarity of my diagnosis cannot be understated. Necrotizing fasciitis, a serious bacterial infection, affects only 0.4 in every 100,000 people in the United States each year, according to the National Institutes of Health. Of those diagnosed with the infection, nearly one in three die.
The symptoms of Necrotizing fasciitis are often generic and easily conflated with other diseases. Body aches. Fever. Chills. Nausea. Diarrhea. Severe pain. As the disease progresses, tell-tale signs — reddened skin, swollen tissues, unstable blood flow, blisters, necrosis, low blood pressure, sepsis — begin to appear.
Late diagnosis can have dire consequences for patients. Because the infection progresses quickly, attacking the skin, subcutaneous tissue and fascia, treatment must begin promptly. Failure to diagnose and treat the infection swiftly causes infected tissue to die, resulting in necrotic (dead) flesh and fascia, which must be removed. Some NF patients undergo amputations. Others become septic and die.
Having never heard of this condition ahead of my diagnosis, I knew nothing of its prognosis.
From ED to ICU
Upon coming to the emergency department, I was certain I knew what would happen. I’d be given a prescription for an antibiotic, I thought, and perhaps something for the pain, then be sent on my way.
After receiving the Necrotizing fasciitis diagnosis, and subsequently testing positive for COVID, it quickly became apparent that I was going nowhere any time soon.
I was immediately placed on intravenous antibiotics and admitted to the hospital’s ICU.
From here, things get a bit fuzzier.
I remember my ICU room being inundated with numerous residents, attendings, hospitalists and specialists. A surgeon came through the door, explaining that I’d soon undergo a series of exploratory surgeries to rid my body of necrotic tissue caused by the infection.
More CT scans were ordered. One doctor educated me on my injured kidneys, a co-condition I had acquired as a result of the NF infection. Another informed me that I had sepsis.
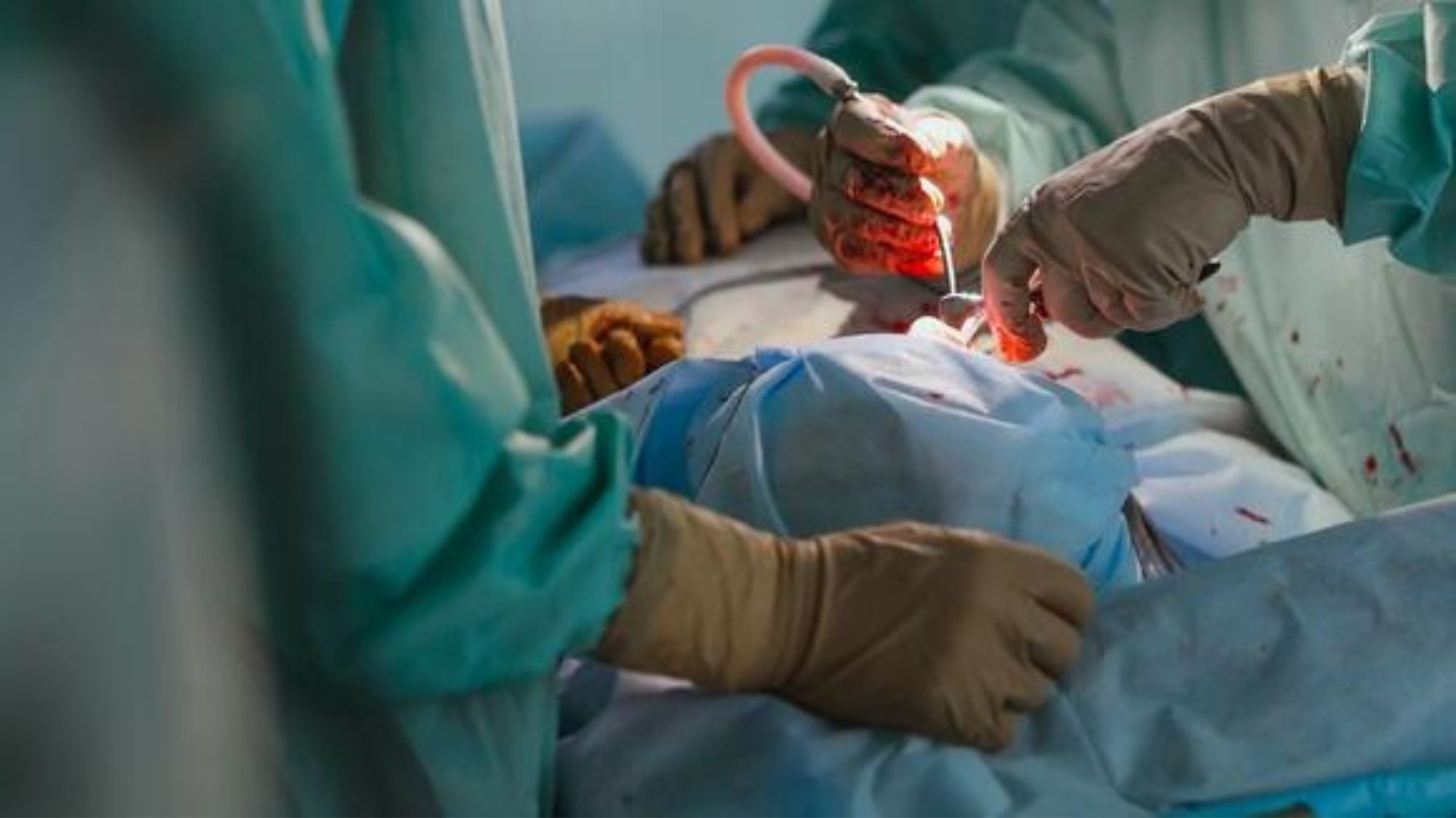
A flood of nurses and nursing assistants and phlebotomists rushed in and out of my room, attaching wires and monitors and tubes to my body. Machines were beeping. My glasses were removed. I was whisked to the operating room. Bright lights and blurry, masked faces awaited me. I was out before I could even begin counting.
A series of surgeries
When I finally awoke, I had no idea what day it was. I had just been roused from a several-day medically-induced coma. My hands were loosely tied to the hospital bed — a precautionary measure meant to prevent me from pulling the breathing tube out of my mouth — and 18 inches of incised skin, left open but bandaged, hung from my abdomen. I was still in the intensive care unit — had been there for nearly a week now — and, at this point, I had undergone several surgeries over many days.
Later, through discussions with doctors and through a review of my surgeon’s operative reports, I’d learn that they’d found “extensive liquefactive necrosis with purulent material throughout the subcutaneous tissue” in my abdomen. The dead tissue, a result of the NF infection, was removed from my body. The wound was cleaned and packed. Thankfully, no amputations were required — an unfortunate consequence of the disease performed on some Necrotizing fasciitis patients.
I had, however, come very close to death.
Further surgeries would ensure all necrosis was eradicated. A wound vac was placed on the opened wound to promote healing from the inside out. (I received no stitches.) I underwent regular physical and occupational therapy during hospitalization. The surgeons and other doctors would monitor me, first in the ICU and then in a trauma step-down unit, while I received daily IV antibiotics over the course of 27 days.
Home to heal
In late January 2023, I was finally released from the hospital. Because of the length of my stay, and because of the effects of the Necrotizing fasciitis on my body, I initially had difficulty walking. I was sent home with a walker and a wound vac. I received twice-weekly home health visits for wound changes and was required to visit the hospital’s surgery clinic weekly for several months.
I've sinced healed well, but still have many obstacles — both in terms of health and in everyday life — to overcome. Treatment for NF, like many long-term conditions, is expensive. The long hospital stay and recovery initially made working, even in a freelance capacity, difficult. Thankfully, I'm now back to freelancing full time.
While I’m proud to say I have survived Necrotizing fasciitis, I’m still susceptible to many consequential long-term complications. I now have an increased susceptibility to infections such as pneumonia, cholecystitis, urinary tract infections and sepsis. And, according to one study by the National Institutes of Health, I’m also now at an increased risk of premature death.
There’s also a large psychological toll to be paid for undergoing such a health scare. I now live in terror of simple rashes and pustules, fearing every bump will lead to another round of NF and, perhaps, death.
Still, I have much for which to be thankful. I’ve still got all my limbs. My health continues to improve.
Most importantly, I’m still alive, here to tell my story and educate others about this very rare and very deadly disease.